|
Located in Front Royal, Virginia, the Shenandoah Valley Family Practice Residency is a medical practice and residency program affiliated with the Medical College of Virginia and Virginia Commonwealth University School of Medicine. Shenandoah Valley Family Practice Residency specializes in training doctors to navigate the challenges of providing medical care in rural areas.
According to research published by the National Library of Medicine, roughly 20 percent of Americans live in rural areas, but less than 10 percent of physicians practice in those areas. By 2025, research by the federal government shows rural areas will have a shortage of over 20,000 physicians. Rural areas tend to have older populations and a higher number of health problems. In rural areas, over half of all hospital admissions are patients over age 65, while urban areas see only 37 percent admission of older patients. Rural patients may also delay seeking care due to economic factors, such as needing to work long hours with no time off. They may also have restricted access to specialists, causing ailments to remain undiagnosed or untreated.
0 Comments
Located in Front Royal, Virginia, the Shenandoah Valley Family Practice Residency is a medical practice and residency program affiliated with the Medical College of Virginia and Virginia Commonwealth University School of Medicine. Shenandoah Valley Family Practice Residency specializes in training doctors to navigate the challenges of providing medical care in rural areas.
According to research published by the National Library of Medicine, roughly 20 percent of Americans live in rural areas, but less than 10 percent of physicians practice in those areas. By 2025, research by the federal government shows rural areas will have a shortage of over 20,000 physicians. Rural areas tend to have older populations and a higher number of health problems. In rural areas, over half of all hospital admissions are patients over age 65, while urban areas see only 37 percent admission of older patients. Rural patients may also delay seeking care due to economic factors, such as needing to work long hours with no time off. They may also have restricted access to specialists, causing ailments to remain undiagnosed or untreated. Affiliated with the Virginia Commonwealth University, Shenandoah Valley Family Practice Residency is a rural-oriented program operating out of the Shenandoah Valley in Virginia. The program is certified by the Accreditation Council for Graduate Medical Education. Three members of the Virginia-based teaching faculty have previously received the Virginia Family Medicine Teacher of the Year award -- Dr. Andrew White, Dr. Frank Dennehy, and Dr. Thomas Ball. An area of particular interest to Shenandoah Valley Family Practice Residency is telehealth.
Policy changes necessitated by the COVID-19 pandemic have altered the face of health delivery, and have promoted the use of telehealth by reducing barriers to access. Also known as telemedicine, telehealth employs digital communication technologies such as mobile devices to access and manage health care services remotely. Through telehealth the doctor provides healthcare without the patient having to make a clinic visit. Today, telehealth is used to deliver primary, specialty, chronic, and acute care. Many health professionals endorse telehealth services and are guiding its wider use in this fast-evolving landscape. Early in the pandemic, telehealth surged as providers and consumers sought ways to deliver and access healthcare safely. For example, according to a McKinsey & Company report, overall telehealth utilization in April 2020 for outpatient care and office visits was 78 times higher than recorded just two months earlier in February 2020. Telehealth has great potential not only to increase access to healthcare but improve uptake of services. However, any expansion in the use of telehealth should only be implemented with the clear objective of reducing health disparities and addressing health equity as challenges remain for many communities. Telehealth should have sustainable, supportive policies that facilitate access to end-user devices and broadband if more underserved people are to be reached. It must not be left to lag once the world overcomes the COVID-19 pandemic. Shenandoah Valley Family Practice Residency, located in Front Royal, Virginia, is committed to providing quality healthcare to the local community's residents. A recipient of several awards over the years, Shenandoah Valley Family Practice Residency also takes a particular interest in helping people deal with pandemic related depression.
Besides the devastating impact of the pandemic on the global economy, some of the measures put in place to combat the virus have had adverse effects on many individuals' mental health. Chief among these is depression. Although there have been significant improvements due to the relaxation of these preventive measures, these tips can still be useful in dealing with depression during a pandemic. Stay Busy The lockdown measures put in place to combat the pandemic means that you spend most of your time indoors. Staying busy is a great way to keep your mind sharp and reduces the chances of dwelling on negative thoughts. If you cannot work remotely from your home, consider learning a new skill or indulging in your favorite indoor pastimes. Plan A great way to put your free time to better use is by creating a plan. Consider breaking your day into smaller bits and setting time limits on each activity. To ensure that you do not lose track of time, be sure to set reminders. Reach Out Remaining isolated is a great recipe for depression. Although physical contact should be reduced during the pandemic, experts still recommend staying in touch with family and friends. Consider calling at least two friends or loved ones each day. Shut Out Watching the news right now might not be such a great idea. Consider turning off the TV or switching to more pleasant channels. However, remember that it is essential that you receive regular updates on any lockdown measures and stay current with government health institutions' safety tips.  Located in Front Royal, Virginia, the Shenandoah Valley Family Practice Residency provides quality medical training while caring directly for patients in the clinical setting. Shenandoah Valley Family Practice Residency faculty members have included a VAFP Virginia Family Physician of the Year Award winner and three VAFP Virginia Teacher of the Year Award winners. The Virginia Academy of Family Physicians (VAFP) established these awards to recognize organization members who have set themselves apart through their distinguished professional service and accomplishments. Both Family Physician of the Year Award and Teacher of the Year Award recipients receive a commemorative certificate at the annual meeting of the VAFP. In addition to providing exceptional and compassionate medical care, nominees for Virginia Family Physician of the Year must play a constructive role in community affairs and serve as a positive example in the medical community. Virginia Teacher of the Year candidates must exhibit similar exemplary performance while providing instruction at the medical school, residency faculty, or community preceptorship level 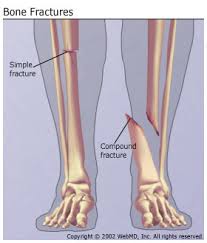 Offering programs in northwestern Virginia’s rural areas, Shenandoah Valley Family Practice Residency emphasizes in-depth, personalized health care training in a variety of settings. Practitioners in the Shenandoah Valley Family Practice Residency program gain experience that includes caring for injuries to limbs. Leg fractures are typically associated with falls and speed-related injuries, where something hits hard and fast. Imaging tests such as X-rays are the first step in identifying the issue at hand and developing a plan for putting the bone’s broken parts back together. In cases where the fracture cannot easily be resolved, artificial rods and screws may also be used in providing proper support and fixing the placement of bone fragments. Once the bones are properly oriented and affixed, they are held in place through the use of a plastic or plaster cast. Typically 6-8 weeks in the cast is enough for the broken bones to fully heal, with crutches used to prevent too much pressure being placed on the leg while it is healing. Keep in mind that sprains can be more serious than they appear at first. In cases where the sprain does not heal within a few days, or the leg cannot bear the body weight and the joint is numb or loose, a torn ligament may be the issue, and physician assistance should be sought. The Shenandoah Valley Family Practice Residency is a three-year program providing doctors with education and practical experience in treating patients of all ages. Those accepted in the Shenandoah Valley Family Practice Residency program learn different approaches to providing patient care.
An article published by a peer-reviewed medical journal, Annals of Family Medicine, discusses the possibility of reducing the transactional functions of physicians and veering toward personalized healthcare to meet the needs of the patients. The article noted that time- and energy-consuming transactional tasks such as data gathering and entry, documentation of care, guideline-based disease management, billing, and even preventive care can get in the way of physicians’ true aspiration: providing individualized care and developing long-term relationships with patients. To make the shift to personalized care possible, changes would need to happen at all levels in medicine, including areas from education to delivery organizations, policies, tools, and payment. Physicians could undergo training and development in personalized care, including oral and written communication skills. Hospitals and other healthcare organizations would need to examine support staffing ratios to accommodate the transactional tasks that would be delegated among medical assistants and other health care personnel.  The Shenandoah Valley Family Practice Residency Program (SVFPRP) is a unique learning opportunity for doctors interested in family medicine, with elective options available for subspecialties including global medicine and obstetrics. In particular, the Shenandoah Valley Family Practice Residency Program focuses on the development of talented physicians with an interest in practicing rural medicine. The state of rural medicine in the United States is causing concern, as doctors in these areas are choosing to relocate or retire, leaving behind a crucial community position to be filled. For residents still considering their career paths, below are three reasons to consider rural medicine. 1. Ongoing learning opportunities. Rural physicians are often expected to serve as a dynamic medical resource for a whole community. They treat illnesses many urban doctors never study, as these cases are often relegated to nearby specialists. Rural physicians are always learning, encountering new conditions and gaining new skills on the job. 2. Assistance on student loan payments. Due to the high need for skill in rural areas, the U.S. government offers state and federally funded loan repayment and reimbursement programs for those who work in rural medicine. In many cases, the longer a physician works in rural medicine, the more financial incentives he or she receives. 3. No job shortages. Rural areas of the U.S. are in desperate need of talented doctors, a problem only sure to grow, as research indicates there may be a shortage of as many as 90,000 physicians in just six years. With the ratio of doctors to patients at one for every 2,500 people in rural areas, physicians who work in these areas will never find themselves struggling to find work.  Located in Front Royal, Virginia, the Shenandoah Valley Family Practice Residency is an accredited program geared toward rural practice. The Shenandoah Valley Family Practice Residency includes a thorough grounding in obstetrical practice for the family physician. Ectopic pregnancy is the most common cause of death in a pregnant patient’s first trimester and affects nearly 2 percent of pregnancies. It develops when a fertilized egg attaches outside the uterus, typically in the fallopian tube. When this happens, the zygote cannot grow, and the mother’s life may be in danger. A patient with this condition often presents with abdominal pain and has missed periods. To determine whether an ectopic pregnancy is the cause, the physician performs a pregnancy test. If the result is positive, the doctor can perform a transvaginal ultrasound, which images the reproductive tract and can determine whether the pregnancy is healthy. If the pregnancy is ectopic, the ultrasound is less likely to prove ectopic pregnancy conclusively and more likely to reveal an undefined mass. Analysis of the patient’s beta hCG hormone levels can usually determine whether this mass is indicative of an ectopic pregnancy, as these hormones tend to rise significantly when a person is gestating.  The Shenandoah Valley Family Practice Residency offers comprehensive training to early-career family physicians, many of whom may wish to practice in rural settings with limited resources. To prepare residents for this kind of care, the Shenandoah Valley Family Practice Residency provides residents with more emergency psychiatry training than is typical for similar programs. When a patient with psychosis presents in the emergency room, he or she requires both medical and psychiatric stabilization. The first step is triage and clinical assessment, which determines whether the patient is in need of immediate medical attention. If no such care is needed, the team must determine if the patient can wait alone for further attention or if he or she needs supervision, a secluded waiting area, or to be placed in a secured room. The care team then moves on to stabilize the patient's psychiatric condition. Typically, the goal of this endeavor is to calm any agitation, reduce disruptive behaviors, and minimize threat of harm to the self or others. Medication, either intramuscular or oral, can help to speed this process, although many experts urge behavioral interventions to be a first course of action. The patient typically then receives a complete diagnostic workup, including thorough evaluation of first-onset psychiatric symptoms. All patients receive a psychiatric evaluation to determine whether the patient is safe for discharge or must be admitted into an inpatient facility or other treatment setting. |
AuthorOverseen by Dr. Frank Dennehy, Shenandoah Valley Family Practice Residency Program offers opportunities for students who are interested in family medicine. Archives
November 2021
Categories
All
|

 RSS Feed
RSS Feed
