 Committed to providing comprehensive training for family physicians, the Shenandoah Valley Family Practice Residency strives to ensure residents' competence in identifying and responding to mental health issues. The Shenandoah Valley Family Practice Residency's curriculum on behavioral health and psychiatry stands out as one of the few nationwide to meet the American Psychiatric Association's recommendations for training in family medicine. If a clinician suspects that a patient has a problem with an addictive substance, he or she may present the patient with four key questions. These questions are known as the CAGE screening tool. Initially created specifically to screen for alcohol dependency, the questionnaire now includes an adapted form that incorporates drug use. The first question inquires as to whether the patient feels it might be necessary to cut down (C) on drinking or use of drugs, while the second asks if the patient has felt annoyed (A) by others’ criticism of his or her drug or alcohol use. The third question screens for any feelings of guilt (G) that the patient may have about his or her use, and the fourth asks if the patient has used alcohol or drugs in the morning as an eye-opener (E) to eliminate a hangover or calm the nerves. A “no” answer results in no points, and a “yes” answer is worth one point. Higher scores indicate a greater likelihood of problems with drugs or alcohol. A score of two or more is defined as clinically significant.
0 Comments
 The Shenandoah Valley Family Practice Residency is a rural-oriented program located in northwestern Virginia. Fully accredited by the Accreditation Council for Graduate Medical Education (ACGME) and the American Osteopathic Association (AOA), the Shenandoah Valley Family Practice Residency Program recently achieved the ACGME's Osteopathic Recognition accreditation. In 2014, the AOA, the ACGME, and the American Association of Colleges of Osteopathic Medicine (AACOM), agreed to the formation of a single system for graduate medical education accreditation in the United States. The new system, which is scheduled to be fully implemented in 2020, will allow MD and DO graduates to complete their residency education in ACGME-accredited programs. Additionally, the system will recognize the unique contributions osteopathic medical professionals have made to the health care industry. The single accreditation system was established to help maintain consistent evaluation standards for resident physicians, eliminate duplication in the graduate medical education accreditation process, provide cost savings for the institutions that currently offer dual programs, and ensure that both MD and DO residency applicants can attend accredited programs. 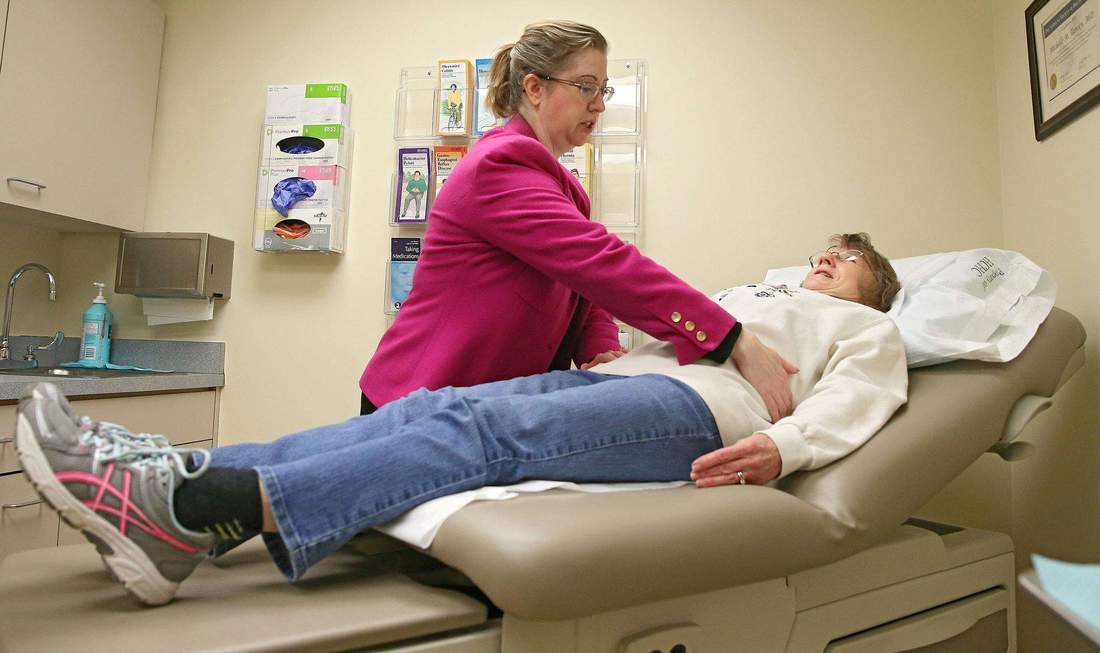 Rural environments require a different sort of medical professional than urban centers. The focus of the Shenandoah Valley Family Practice Residency is to equip new physicians with the skills needed to handle the unique problems that arise in smaller towns. There are one and half times as many primary-care physicians per person in urban areas as there are in rural areas. For specialties like orthopedics, cardiology, and oncology, the number rises to two and half times as many physicians per person. This means that rural doctors tend to cover a wider variety of medical needs and procedures, and need to have broader skills. These kinds of situations and opportunities are what training programs like the Shenandoah Valley Family Practice Residency seek to address. Working in a rural area as a medical professional does have its benefits. The lower cost of living in the country allows for a doctor’s salary to go much farther than it would in a city where rents and mortgages are high, as are the prices of goods. An additional benefit may be lower stress, despite the lower density of physicians to patients. According to one survey, 61 percent of rural physicians have said that the pace is slower at their practices in the country that it was in the city. And doctors in rural areas tend to know their patients better, leading to greater professional and personal satisfaction.  The Shenandoah Valley Family Practice Residency, like approximately 9,600 other United States residency programs, is accredited by the Accreditation Council for Graduate Medical Education (ACGME). The Shenandoah Valley Family Practice Residency is subject to review based on ACGME’s milestones, which are designed to assess the quality of residency programs and facilitate improvements when necessary. Milestones can be seen as developmental outcomes, such as skills, attitudes, and performance, which are competency-based. They were put in place by ACGME along with the American Board of Medical Specialties and residents to help residencies’ educational efforts result in competent and highly trained physicians. For residency programs, milestones assist in creating curricula and designing assessments. They also provide a framework with which to identify residents who may be struggling. Milestones impact residents themselves by providing transparent expectations, supporting self-motivated learning, and improving mechanisms for clear feedback. In terms of the ACGME’s accreditation efforts, the milestones increase public accountability and enable continuous program monitoring.  Based in Virginia, the Shenandoah Valley Family Practice Residency program is an ACGME and American Osteopathic Association-accredited residency that focuses on providing physicians with the tools they need to practice rural medicine. If new medical school graduates are looking for a meaningful educational experience, they might consider applying to the Shenandoah Valley Family Practice Residency program for the following three reasons. 1. Training in both small and large-scale medical settings: Many doctors never receive the opportunity to learn about practice in a rural area. To help prepare medical professionals for a variety of unique rural health situations, this program educates residents in diverse settings, from the 411-bed Winchester Medical Center to a small, local practice and hospital in the town of Front Royal, Virginia. 2. Rural patients’ need of proper health care: Rural doctors only make up only about 10 percent of all physicians, which means that Americans living in rural areas do not get the same range of health care options as their counterparts in the city. Participating in a program designed for rural doctors means the physician will be helping to fill an important need in disadvantaged communities. 3. Access to the outdoors: The program is situated near several major parks and forests, including the Shenandoah National Park and the Appalachian Trail. Medical professionals interested in living an active outdoor lifestyle will find plenty of ways to keep busy during their educational experience. A three-year, rural-orientated program, Valley Health’s Shenandoah Valley Family Practice Residency uses training sites in both Front Royal and Winchester, Virginia. As an indication of the program’s high standards and reputation for quality, several residents of the Shenandoah Valley Family Practice Residency have presented at the annual conference of the North American Primary Care Research Group (NAPCRG) for three years in a row.
Established in 1972, NAPCRG is the largest group of its kind in the world. With members representing behavioral sciences, health services research, and all of the health care generalist disciplines, the nonprofit organization is dedicated to spearheading practice-based research networks, funding a wide range of research projects, and connecting its members at annual meetings. Led by nine different committees, the organization recognizes research innovations and significant achievements in the field with its awards and scholarships, including the Maurice Wood Award for Lifetime Contribution to Primary Care Research and the Distinguished Research Mentor Award, among others. Presented at NAPCRG’s annual meeting, the Distinguished Research Mentor Award recognizes a member for his or her contributions to the field. The award is open to researchers who are current NAPCRG members with at least 10 years of related professional experience. Additionally, applicants must be nominated by someone who is also a NAPCRG current member. Award qualifications further include a letter of support and a summary of the nominee’s mentoring work. Other awards NAPCRG issues recognize distinguished work of trainees, student research, and new investigators in the field. Through the Shenandoah Valley Family Practice Residency, early career doctors (resident physicians)have access to a thorough curriculum in behavioral health and psychiatric care. The Shenandoah Valley Family Practice Residency is one of the few such programs in the nation to meet the American Psychiatric Association's recommendations for family medicine training in practical psychiatry for later practice.
According to a survey conducted by the American Academy of Family Physicians, approximately 18 percent of individuals seek treatment for a mental health disorder over the course of a year, and 52 percent of those seek such treatment in primary care. The academy has also estimated that as many as 36 percent of patients in primary care have a psychiatric disorder, which means that family practitioners must have a competent understanding of and sensitivity to emotional distress. The American Academy of Family Physicians' specific competencies for mental health knowledge include the understanding of normal human development and its relationship to patient care. Practitioners must also be able to knowledgeably evaluate patients for mental illness, refer a patient or begin treatment as appropriate, and provide interventions in emergent psychiatric situations as they arise. Overall, the family physician must develop an understanding of the relationships between mental, physical, and social wellness as they apply to the comprehensive health of the patient. Based in Virginia, the Shenandoah Valley Family Practice Residency program is a fully accredited residency program available to medical professionals, one of a few of its kind that serves rural areas of the country. For many years, the Shenandoah Valley Family Practice Residency has participated in the North American Primary Care Research Group's (NAPCRG) Annual Meeting, submitting projects accepted at the event, as many as 10 research projects in the last three years.
NAPCRG's Annual Meeting is held each November in a different city. Professionals in medicine worldwide gather at the meeting to hear panels and lectures, watch colleagues' presentations, and discuss the latest developments in primary care research. Each year, the organization has a call for papers, where participants can propose a category or topic regarding primary care research to present at the meeting. Similarly, there is a poster session for researchers, where participants can submit a poster that concisely sums up his or her research in the field and give a presentation that includes handouts or business cards, opening up opportunities for networking. Founded in 1972, the NAPCRG is made up of professionals from several primary care disciplines and related fields. For more information, visit www.napcrg.org. |
AuthorOverseen by Dr. Frank Dennehy, Shenandoah Valley Family Practice Residency Program offers opportunities for students who are interested in family medicine. Archives
November 2021
Categories
All
|
 RSS Feed
RSS Feed
